Using Big Data to Manage Health
| Project Infobox | |
|---|---|
| Self researcher(s) | Michael Snyder |
| Related tools | apple watch |
| Related topics | Genome and microbiome, Metabolism, Blood tests and blood pressure, Saliva, Personal genome, Personal microbiome, Blood glucose tracking, Cholesterol |
Builds on project(s) |
|
| Has inspired | Projects (0) |
| Show and Tell Talk Infobox | |
|---|---|
| Featured image | 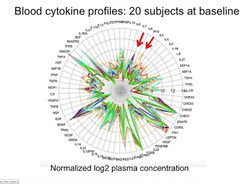
|
| Date | 2017/03/15 |
| Event name | Bay Area Meetup |
| Slides | |
| This content was automatically imported. See here how to improve it if any information is missing or out outdated. |
Using Big Data to Manage Health is a Show & Tell talk by Michael Snyder that has been imported from the Quantified Self Show & Tell library.The talk was given on 2017/03/15 and is about Genome and microbiome, Metabolism, Blood tests and blood pressure, Saliva, Personal genome, Personal microbiome, Blood glucose tracking, and Cholesterol.
Description[edit | edit source]
A description of this project as introduced by Quantified Self follows:
Mike Snyder runs a lab at Stanford focused on finding predictable patterns of potential disease or sickness in ones body by using a huge amount of data. Basically, they are looking for an individual’s healthy state at a personal level and what happens when they transition into other states (i.e. sickness or disease). Mike shares his personal story and data of going through 10 viral infections, Lyme disease and a bike accident. Then, he discusses the sequencing of his genome, which predicted many things that matched his family history, including that he was at risk for type 2 diabetes that he got during the course of the study.
Video and transcript[edit | edit source]
A transcript of this talk is below:
Using Big Data to Manage Health by Mike Snyder
Some of the work we’ve been doing for the past 20 years is different kinds of data and in our case for really understanding health and seeing what happens when you transition to disease. Now, this is really frames of thinking that goes on in our lab. We like to try and think of it can be health, it can be other things. But you are in a state, hopefully, healthy most of the time but you can transition into times when you're not healthy or stress or other sorts of states. And it's influenced by many different variables. Obviously, your DNA is one of these variables, but there are many other sorts of things as well. Pathogens, food, stresses, etc. can all contribute to your stat. And so, I would argue, certainly ion our lab and in many others and probably a lot of people in this room and try and see this is quantitative terms, I really do believe that we will be born in the future, not us but our successors will be born with their genome sequence, and we'd like to understand in the presence of what other kind of variables you can predict what kinds of health or disease or stress outcome states you'll be in. So many of you may know it turns out now seven years ago this month we set up basically deep data approach, with the goal of essentially trying to define what is a healthy state or what happens when you transition into these disease states. And so, I won't go into these details too much, but we now do 14 different Omics. So sequencing your DNA, your genome is one of the Omics. But then we also look at your epigenome for – not sure how many biologists are here. How many are not biologists I guess I should ask? In fact, it's very clear for example, exercise will directly lead to the modification of your DNA, which probably affects your geneome. So anyway, we are studying epigenome, is the one we’re studying is ethylating your DNA and modifying it. But we also look at all your RNA, that’s your transcription, your propodeum as much as we can. This is mostly out of blood components, cytokines are very important immune modulators, and we try and follow as many metabolites as possible. We follow thousands of these that we know of and many other peaks and lipids as well, and these are all very important. We can actually follow your antibody reactivity to any antigen you might have in your human body as well as the whole common virum that we can see what viral activity you have. From your serum, we do follow five different microbiomes or collaborating with u-biomes 0n some of this. We've been doing quite a bit already the stored gut microbiome and nasal, and we're just adding on some of these others as well. And then recently in the last few years, we've added on biosensor measurements, and I thought I'd spend quite a bit of time on that since it seems to be a very popular topic. And we did this longitudinally over time, so we're following people on a sample regime, and I tell you about that in a minute. But the idea is to get these longitudinal measurements because I think that's really the power of what I'm about to tell you. And all of them by the way were making literally I should say not automatically, we make billions of measurements every time we sample someone. So again, most of this is out of blood, the metabolome, the lipid mixture out of blood and urine and the microbiome from surrounded parts. And so there are many goals of this study, but simplistically put what we’re trying to do again is to find at a personal level what is an individual’s healthy state, what happens when they transition into other states. Disease being one of the obvious ones, but what happens when you get a colonoscopy, or you change your diet, or you go to Malaysia, things like this. These are all situations that we want to try and understand at a personal level. And along the way, we identify things that turn out to be important for people’s health as you’ll see in a minute. So many of you may know, and again we started this on me, it turns out seven years ago. It was really meant to be a proof of principle to get the technology going. And since that time we’ve started, I’ve been through 10 viral infections, Lyme’s disease, a big bike accident last summer when I woke up in a hospital and that sort of thing. So we make the best of these adverse situations, we sampled me about every 2 to 3 months when I’m healthy. But when one of these interesting times like a viral infection comes we take many many more samples. So a very typical one, these are day numbers here into the study, but these are all very common cold viruses if you will. HRV means rhinovirus, that’s the most common. Here's nine months into this study, I actually got a respiratory sensational virus infection that we do. And again you will see very dense sampling during these periods, and then again back to when I'm healthy, and you’ll notice a whole bucket load of sampling going on. And that’s been going on for the last two years because I’ve been doing different dietary prohibitions, trying different fiber supplements to see with their impact on my various Omics and on my health, and those are some of the things you will see. So I'm going to through this part and bit quickly to just give you a feel. We started by sequencing my genome, which predicted many things much which matched my family history. And to make a long story short, one thing that I was not aware of is that I was at an increased risk for type II diabetes. And because we were measuring glucose, which is a metabolite and as I said we do all of the standard medical tests as well. Once you know it during the course of the study, in fact, I got type II diabetes. So my glucose was marching along perfectly normally, and then ironically when I went in for a very fancy glucose metabolism test that came out elevated, we were both surprised. Tested it again – this is just my fasting glucose. It's this number here, it's quite high, and it's not normal. And then a week later it was even higher, and it's arbitrary, but hemoglobin A1C is a measurement for steady-state glucose, and it’s arbitrary. But diabetes is classified as 6.5, and I was right at 6.4. So right on the edge, so five weeks later I went to my general practitioner, measured me again, glucose even higher. Hemoglobin A1C 6.7 and classified as diabetic. So the bottom line was that in fact, I became diabetic during the course of this. I change my diet, I doubled my biking and started running, and that's about eight months to bring me back down to normal. So this made a big deal at the time because it was the first time someone use their DNA to predict the disease and I got the disease, and in my case it was manageable. At least temporarily you will see. And it's also fascinating for many scientific reasons because what we think is going on, you will notice that this spike in glucose came right after this nasty viral infection. Now the viral infection lasted a few days, but my glucose was elevated for eight months and took quite an intervention to bring it under control. So some people say, well maybe Mike that would have gone away on its own, so we accidentally did the right experiment. Which is when we scaled which you will see in a minute, to 100 people we kept this going, but we weren’t looking at the data. So effectively I was blinded if you will from the data that was coming in. And then right around here, someone looked at the data and said Mike do you realize your hemoglobin A1C is 7.0 again, you’re diabetic. I said no, I had no idea. Sampled me a few more times. I forgot to say I stopped running right around here. Started running and brought it down, but it’s been creeping up. This chart is about two years ago, and it’s been creeping up ever since in fact, over the last several months my hemoglobin A1C is 6.7 again and I’m back in the diabetic range. So, there is no question that I have a glucose miss-regulation problem. And it turns out that my brothers and sisters we sampled as well, and they all have the same problem. So what we think is going on is that I'm genetically predisposed, and then there are other factors that contribute to this. And in this case, I forgot to mention I think probably the viral infection triggered the disease, and that's a hypothesis anyway, it's an association and not necessarily causation, although, anecdotally lots of people had similar situations. So as I mentioned, we are now scaling this to many others, so what we are doing exactly for them is what we’ve been doing to me, and this has been running for about four years now. So every three months we sample them when they’re healthy, and then when a viral infection, stress response which took people up 48 hours we would sample them after that. Seven people have been through colonoscopies, so we do many samples after that to see their effect on what their health profile looks like if you will. And then we’ve also been running all kinds of dietary studies as well. Some people doing weight gain, weight loss studies. A lot of different fiber supplement kind of studies as well. And I won’t have time to go through all of these, but it’s quite fascinating. And again we do dense sampling during this time. Now what’s special about this and this will be something for this group to think about how to organize data, especially that’s been collected by uniformed devices. What’s special about our group is that they decided nearly all agreed to make their data completely open. Minus days and birthdays, so scientifically this is an incredible valuable data set, and you can start downloading. Some of it is up there already, and by summer we'll have just a ton of data, and I hope a petabyte or two of data of all these different sorts that'll be out there for analyzing. This slide, by the way, is a year old, and so there are 1000 datasets that are time points that'll be analyzed in detail by summer, probably more than that, and we've got over 50 people with many many more samples. Again they are longitudinally samples, so we think it's a very powerful dataset and very unique. So again I don’t have time to run through this, there’s a zillion interesting vignettes here, and are just tell you a couple of them. This is a genome story, so 60 people have had their genomics sequenced, and then analyzed in excruciating detail. That takes a lot of work. It takes one person around 40 hours to go over a genome the way we go over it. It’s not your typical genomics analysis. And it turns out that 11 of these individuals have information in their genome that affects their health care. That is to say, there is a mutation, and they have a variant that puts them at higher risk for a disease, and because of that, when they go to a doctor's office they will be tested for this. So the net result is even though this is a minority; it's 11 out of 60 if you're one of those 11 it's a big deal because, for example, two people out of this mutation of this gene put them at higher risk for a paraganglioma. So this is a simple urine test, and it's not a thing you do performatively. This is a very interesting one; this is a male who has a BRCA mutation, which does put him at risk for breast cancer even though he's a male. He obviously won't get ovarian cancer, but he has two sisters. So what does he tell his sisters about his genetic condition? These are some of the issues that are out there. They can tell you a lot of this stuff is really powerful, like this one here, it's a particular kind of mutation. This person has elevated glucose, but he was thought to be a Type II diabetic or nearly type II diabetic. But his mutations suggests he's a different kind of diabetes, and the treatment for this individual is very different from a normal Type II diabetic. So the information from this world changes treatment. He is not diabetic yet, but he's on his way. Age is a normal factor, so he will probably get a different kind of treatment. This is the kind of stuff that you can get, and this person turns out has some heart issues. So anyway, this is what you can get from your sequencing data and one thing you can all enjoy we can do things like these cytokine profiles. Cytokines for those of you who don't know, these are important immune molecules. They regulate your immune system, and everybody has a different baseline level and a different healthy level, so nobody is the same. So each color is a different person, and these are 63 sets of cytokines and growth factors, so the blue person has high levels of AL7 and so on and so forth. And we think this is what makes us susceptible to different diseases. A lot of this is probably epigenetic, actually not genetic so there is a few that’s genetic. So as I mentioned, we're recently we've been bringing in the wearables, so we've tested – in the summer of 2015, we did a census where there is over 500 health-related wearable devices. We tested about 30 of these and settled on at least well a number of those. I use eight of these devices every day, and some of them are on the slide. And the bottom line is that the measure many many different things. Actually, how many of you are wearing a wearable right now? I assumed it would be 100% but it’s not. Okay, that’s the almost Quantified Self, all right. Anyway, so they measure steps and activities, and a lot of these are free apps on your phone. They will drain your battery, but there is no other cost to you to actually collect this information. And there are all sorts of things, heart rates, skin temperature, stress response, which is conducted to your skin and so on and so forth. Even your, you know, you can get your weight registered on your scale and nearly all this information, not all, will transfer to your iPhone. I should say that this study, it was really led by Chow Lee, whose somewhere in the – and there she is on the back and also Dahlia, whose on a different aspect of this study. And then we have others as well, who I’ll mention, Jesse Dun, and Dennis Alland are particularly really terrific. So for some of the stuff you think is strange, like the radiation monitor, and it is strange but has interesting results. So anyway, this shows what a profile looks like, and many of you are probably familiar with this. This is my profile. So the top is sleeping, so it shows when I sleep. I sleep at night and I’m awake during the day so no surprise there. These are for my non-travel times. This is my heart rate, yet low at night and up during the day, as is my resting heart rate. This is skin temperature. Higher at night, and this is a little different from your core temperature, higher at night and lower in the days. So you can see you get these personalized baseline parameters. We not only do this for me is, we do it for others, and this, this parameters are 43 other people. Everybody has a different baseline heart rate and the different skin temperatures. None of this is a surprise, but the point of all of this is this is to get people’s individual baseline measurements. Everybody has again, personal baseline activities, which we grouped them into four classes. So this is a pretty typical one. There are people, again, not active at night and relatively constant during the day. It might just be that they are desk sitters, couch potatoes or whatever during the day. But there are other people who are morning people. You see these single spikes in the morning, and others that are kind of two humped camels, morning and afternoon, and three humped morning, afternoon, and evening, so some people with some different activity patterns. Again, all of this is to define people’s baseline. So where it gets interesting is where you start to try and find deviations from baseline. And this is one example, this is one of my personal examples, but you will see this is true for many others. I treat everyone. So actually this is on airline flights, and it turns out that your blood oxygen drops on airline flights and this is known already. So this is a short flight, this is altitude in green. This is my blood oxygen in blue, and we have continuous monitors now. So it will start out highs, goes low, and then cabin is pressurize at 8000 feet and comes back up and returns to normal. I think what was interesting to us is how much of the flight, which I couldn’t find so well to quantify, 70% of the flight is 96% or below and the relevance of that I say in a minute. Even at 5% is 90 or below and that's something over all the flights, and you can break this down differently for different flights. So it turns out that this wasn’t just true for me, it’s true for every single person, across every ethnic group we looked at which is many as we could find. And I won’t go through the details of this, but green, is people on the ground if you will, blood oxygen and the plane has a blue person. Again everyone’s oxygen drops, assuming the flight is high enough and was long enough, your oxygen will grow on a flight. This is again known already. What was new that we couldn't find any way in the literature is that when the oxygen goes down, it's associated with fatigue. So it doesn't prove causation, but what we found from my personal profile, so 96 and below – there are many exceptions, but 96 or below I'm tired. If you do a blind study where you score that you’re tired and look at oxygen and keep it. And then if it’s 96 or above, this is on flights and in other situations, if it’s 96 or above then I’m generally not tired. 96 is roughly a threshold. All right, we can do a reaction time test for this, meaning this is my level of oxygen, this is my response time in a simple visual reaction time test. And the bottom line is as you can see, as your oxygen drops, your reaction time is slower. So again, what we think what is going on is that when your oxygen is low, you're tired. And so when you see people sleeping on aircrafts, what we think it's not because they have been staying up too late working too hard or what have you, it’s because the oxygen is low on aircrafts. So that’s the association that we made, which again I have not seen in the literature. Some good news is that if the flight is long enough you actually adapt. And for me, that seems to be seven hours. We don't know how general this is yet, but after seven hours, you will see this is a long flight. It starts out here, goes down, comes back up and the whole last part of the flight is much higher than the beginning of the flight. So let’s hope for you who are workaholics, at the end of the flight you might be able to rescue some of that work you promise to do. Why is all this important? Well, we're always looking for deviations from baseline, and there is a very interesting perturbation experiment, it turns out that on one of my flights some of you may have heard this. I was flying through Norway, first through Frankfurt and the last flight is a very short flight, which should have a fairly modest drop in oxygen. So this is my normal drop in oxygen for a short flight. What turns out on this particular flight, you can see that my median was about 90, pretty low right, especially for a short flight. When I got landed, it didn't come back to normal. Not only that, my heart rate and later I learned my skin temperature was high. So this is complicated, but these are outlying measurements. It was looking over a two-year period, and this is when I landed initially, and this is actually several days. And the bottom line is I had a lot more outlying measurements, and it turns out my median measurements are different for both heart rate and skin temperature, and so that actually led to the clues that something was not right when I landed in Norway. Well, it turns out that I got a low-grade fever after that. I went to a doctor there, and I suspected it was Lyme's disease because two weeks earlier I was in Massachusetts. And when I went to a doctor there he took my blood and he said your monocytes are up and I've got a bacterial infection. And he said well, I think you should take penicillin. And I said no, I think I should take doxycycline, which is what you use for Lyme disease. And as you imagine I was a little bit tense for a few moments there. He did give in because they didn't want to be sick above the Arctic Circle, which is where I was going next, and he gave me doxycycline, and I cleared up. And when I got back I did the test for Lyme disease, and I was positive. And I have the perfect control because just before I had left, I had given blood because I give blood a lot, and sure enough I was negative then. So the bottom line is I had Lyme disease, and actually, this was the first clue that tipped me off that something was wrong. Again, because my oxygen wasn't right, my heart rate was wrong. I can show you more of these, and we can look at outliers of heart rate and skin temperature. These are the Lyme disease days. You can't miss them. They're way out outliers, but it turns out that I have other days as well. It turns out that those are other days when I had a standard cold, and I was sick by more of a standard method. And in fact, every time I was sick it gives an outlying measurement on this. And there was even one time that I didn’t realize that I was sick but actually I had high – it’s the only other time I had high heart rate and skin temperature outlying. And then we went back and looked at my measurements. It was blood test that you can do if you’re sick, it’s called CRP. It turns out that was very elevated just like I was normally sick. So the bottom line is, every single time I was sick it was picked up by my smart watch. I see them write some algorithms to try and detect the earliest times when you get sick from your smart watch. We have three other people, I won’t go through the details of this, but the bottom line is we looked for this elevated heart rate over a prolonged period with the low false positive rate. And the net result here is there is three other people that got sick during our study, who had smartwatches on at the time. We can pick up every one of those, and by this one person got sick twice and we picked up theirs as well. So again, now I should point out to people the skin temperature was elevated and two others that wasn’t the case, and all people’s heart rates were high, so we don’t know why the skin temperature is. It might be how they are wearing the device, there some technical issues. But the bottom line is that heart rate wasn’t pretty – we think will be an inaccurate measure for determining these outlying times. I’ll go on to say that I don’t have time to present this, but we think that it starts picking up differences in people’s insa resistance, which is a precursor for type II diabetes. I can explain that more in the questions, but we can see these by outlying heart rate parameters as well. So we think these devices will ultimately be powerful for telling the early stages of type II diabetes, all from your simple smartwatch. So ultimately, I think again your smartwatch is going to be in fact your health nexus of the future. It will become your dashboard just like your car we hope, and that's what we're going to try and do now and make that your dashboard for health. And then we want to try and figure out how to get this to physicians, so they can use this information to help manage your health, and hopefully they won't work – well she's studying intensely that's good. Not looking perplexed, that would be bad. Anyway, this is the future that we’re trying to realize, and I think the Quantified Self is an absolute critical part of this. But I think we are going to be in a world where people’s genome is either sequenced before birth or some of you will get it after birth, and then we’ll have other kinds of information that will be better and that will be used to better manage your health and see these disease transition times. I think I went over, so I won’t spend much time, but I think we are here in terms of personal genome sequencing. I think the most important part of this study is the longitudinal aspect. Understand your healthy baseline, find deviations from that. Not unlike what Carl said and not unlike other speakers today. Try and always see your deviation from your baseline. And I do think wearables will be an important part of this, and I think this crowd might appreciate this too, but I think at the end of the day you’re more responsible for your health. And your doctor will be your doctor. Your doctor cannot understand you the way that you can understand yourself. And so I think this information will be valuable for that.
I just want to credit, and I had an amazing team of people work on this over now again seven years. And so the leaders right now are Wenyu, Brian Piening, Kevin Contrepois and here are all the folks doing all of the wearable studies down here. And again, wonderful collaborators at many levels, and here’s a shameless plug for a book that we had come out.
About the presenter[edit | edit source]
Michael Snyder gave this talk.